So, If you have been diagnosed with Polycystic Ovary Syndrome, you may well have heard of Metformin for PCOS. And while this is one of the most commonly prescribed drugs for women with PCOS, there are some reasons that we you may want to reconsider taking Metformin.
But before we get to that, let’s like at what Metformin is and why might it be prescribed for someone who has been diagnosed with Polycystic Ovarian Syndrome.
What is Metformin?
Metformin (also known as Glucophage) is commonly prescribed to people with Type 2 diabetes. It comes in two forms: an immediate release form or an extended release.
How does Metformin Work?
Well, Metformin works in a number of ways, all of which work to lower blood sugar levels in the body. There are 3 ways in which Metformin works (1) :
- It lowers the amount of glucose that is produced by the liver
- Metformin lowers the amount of glucose absorbed by the body
- It makes your body more sensitive to insulin and improves insulin resistance
Now, you may be prediabetic or have full blow diabetes mellitus. In that case, Metformin would make sense. But why on earth would you want to take Metformin – an insulin sensitizer – for PCOS?
What is the Link Between PCOS and Insulin?
Researchers aren’t sure what causes PCOS but they have shown that insulin is at the heart of the problem. You see, women with PCOS tend to have high insulin levels (Johnson, N 20141). And our ovaries are particularly sensitive to insulin, causing us to have high levels of testosterone.
Now, before you tell me that insulin doesn’t matter because your body mass index is in the normal range, insulin has been shown to be problematic is women with PCOS, irrespective of their weight.
So, if insulin and insulin resistance is at the heart of the problem, then taking something like Metformin may make some sense.
How does Metformin help PCOS?
Metformin was first prescribed for women with PCOS in around 1994 (Lashen, H, 2010 2). At the time, studies and randomized controlled trials showed Metformin treatment resulted in an improvement in the regularity of the menstrual cycle and a lowering of testosterone levels. There are other studies that have shown that Metformin can help prevent gestational diabetes mellitus, help with weight loss, restore ovulation and reduce the risk of miscarriage.
What dose of Metformin for PCOS?

Once you have built up a tolerance and are coping well, you can increase that dose by 500mg every week until you reach a maximum dose of 2500mg per day, depending on the severity of your symptoms2.
Having said that, the average Metformin dose for PCOS is 1500mg to 2000mg daily (2).
Seems like there may be something here that would make Metformin therapy worth considering. BUT, before you run to your doctor to ask for a prescription, I think we need to look at the bigger picture.
Six Reasons to Reconsider Metformin for PCOS
The Side Effects of Metformin Can be Rough
A lot of the side effects of Metformin can be pretty difficult to cope with, especially when you first start taking it and are building up your tolerance to it. Some of the most common side effects include (3):
- Physical weakness (asthenia)
- Diarrhea
- Gas (flatulence)
- Symptoms of weakness, muscle pain (myalgia)
- Upper respiratory tract infection
- Low blood sugar (hypoglycemia)
- Abdominal pain (GI complaints), lactic acidosis (rare)
- Low blood levels of vitamin B-12
- Nausea
- Vomiting
- Chest discomfort
- Chills, dizziness
- Bloating/abdominal distention
- Constipation
- Heartburn
If you are struggling with any of these side effects, you need to speak to your doctor and seriously consider if the benefits are worth the discomfort caused by the side effects.
Long Term Metformin Use can Lead to a Vitamin B12 Deficiency
There are a lot of women with PCOS who were prescribed Metformin years ago and continue to take it. There is a problem with that, however.
You see, long term Metformin use can lead a vitamin B12 deficiency. And this can have some serious side effects (4).
- Weakness, tiredness, or lightheadedness
- Heart palpitations and shortness of breath
- Pale skin
- A smooth tongue
- Constipation, diarrhea, loss of appetite, or gas
- Nerve problems like numbness or tingling, muscle weakness, and problems walking
- Vision loss
- Mental problems like depression, memory loss, or behavioral changes
I have previously written an article on the this Vitamin B12 deficiency caused by Metformin. Why not check it out if you want to know more?
Diet and Lifestyle Changes Trump Metformin for PCOS

The thing is, dietary and lifestyle changes are ALWAYS the first line of treatment for women with PCOS. And if you have been prescribed Metformin, it should only be taken alongside diet and lifestyle changes anyway (Johnson, N 2014) .
In fact, a study looked at 343 obese women with PCOS who were struggling with fertility (Karimzadeh et al. 2010 3). The researchers divided the women into 4 groups with 4 different treatment approaches:
- Clomiphene Citrate
- Metformin
- Clomiphene and Metformin
- Diet and Lifestyle changes
They looked at pregnancy rates in each of these groups. Wanna guess the percentage of each group that got pregnant?
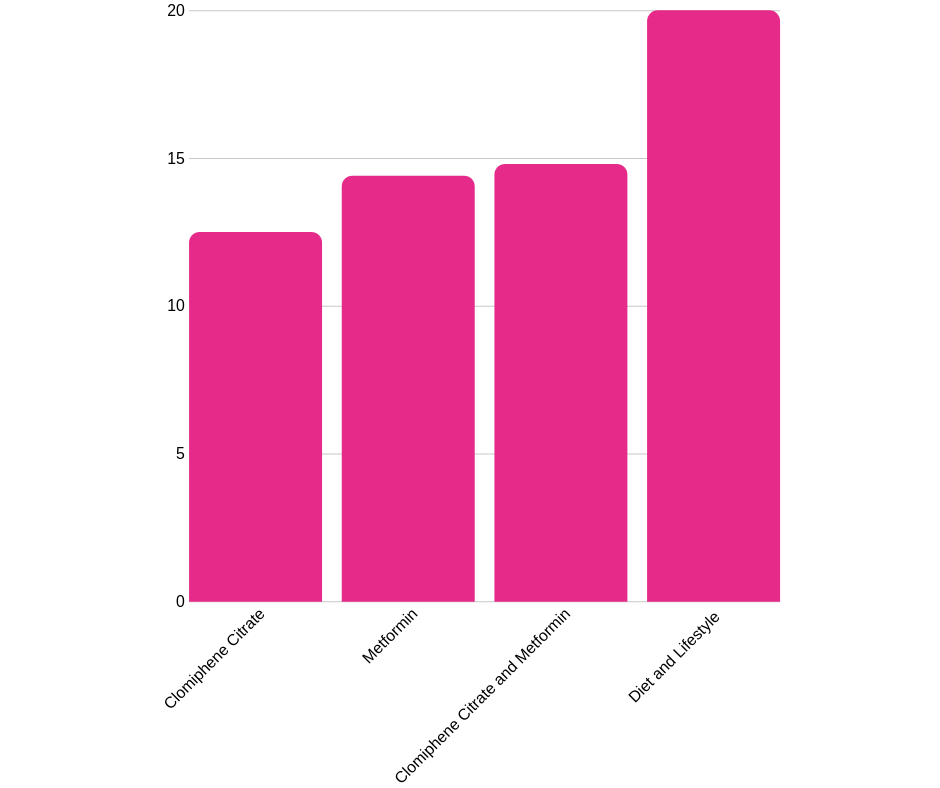
- Clomiphene Citrate – 12.5%
- Metformin – 14.4%
- Clomiphene and Metformin – 14.8%
- Diet and Lifestyle changes – 20%
That is huge and really proves that diet and lifestyle changes are more effective than Metformin in managing PCOS and dealing with a lot of the unpleasant symptoms.
Metformin isn’t the Answer for Weight Loss

Studies have also shown that those women who lost weight while taking Metformin were those women who also made those all-important diet and lifestyle changes too.
Metformin on its own will not help you lose a lot of weight. In other words, if weight loss is your primary concern and the main reason for taking Metformin, you may want to reconsider that decision.
Metformin is an Endocrine Disruptor
Metformin is the most commonly found drug in water and waste systems around the world. And here is the scary thing – it is an endocrine disruptor. Studies have found that this low-dose exposure to Metformin changes the sexual characteristics of aquatic animals, creating intersex fish (Niemuth, NJ; Klaper, RD5). Intersex means that there are fewer defining sexual characteristics between male and female.
Now you might be wondering what this means for you.
Well, if Metformin is changing the sexual characteristics of fish (Maclaren et al. 20186), imagine what it might be doing to our own hormone systems or those of our children.
We may well be trying to fix one problem (our PCOS symptoms) but we’re actually creating another problem of potentially epic proportions.
And given the fact that dietary and lifestyle changes are more effective than Metformin anyway, shouldn’t we go that route instead of ingesting high doses of a known hormone disruptor?
Metformin Isn’t the Best Choice for Infertility

And boy am I glad that I didn’t come away with that prescription!
An article recently published in The Cochrane Database of Systemic Reviews (Morley et al. 20177) recently showed that Metformin is not superior over other drugs in stimulating ovulation that results in a live birth. It seems that Metformin may be helpful when combined with Clomiphene Citrate but it is not superior to Clomiphene.
We are going to talk about natural alternative to Metformin next and my gut feel would be that if you are trying to conceive with PCOS, either Berberine or Inositol is preferable to Metformin to stimulate ovulation and ultimately conceive.
Natural Alternatives to Metformin
The good news is that there are a few natural alternatives to Metformin.
Inositol for PCOS
Inositol has some wonderful effects on PCOS and there is some solid research behind its use. It can help women with PCOS in a number of ways:
- Increased progesterone
- Increased SHBG (sex hormone binding globulin) – Deals with any free testosterone in our blood stream
- Lowered testosterone levels
- Improved insulin sensitivity
- Decreased luteinizing hormone
- Induced weight loss (that sounds good to me)
- Effective in managing hirsutism
- Ovulation induction
There is also some good research on how myo-inositol helps with fertility and pregnancy (Regidor et al, 20188). Inositol has been shown to:
- Restore normal ovulatory activity and fertility in women with PCOS
- Improve egg quality and pregnancy rate in women with failed IVF
- Improve pregnancy rate and lower cancellation rate in women with PCOS
And the amazing thing is that you can get a lot of the benefits of Metformin without the unpleasant side effects. In fact, a recent systematic review of studies comparing the effects of myo-inositol with Metformin showed that Inositol is preferred over Metformin for PCOS (Facchinetti F, et al, 20199). This is mainly because you don’t get the unpleasant side effects with Inositol.
Ovasitol is my favourite brand of Inositol for PCOS.
Berberine
Berberine is a chemical that is found in certain plants and is often used in Chinese medicine. It has similar effects to that of Metformin.
And a quick Google search will give you a lot of the benefits of Berberine but let’s look specifically how it compares with Metformin.
The European Journal of Endocrinology published a study that compared the effects of Metformin and Berberine in 89 patients with PCOS and Insulin resistance (Wei et al, 2012)10.
They found that Berberine lowers
- Total testosterone
- Free androgen index
- Fasting glucose
- Fasting insulin
And increases SHBG (sex hormone binding globulin).
What is also amazing is that berberine is even better than Metformin in lowering BMI and improving cholesterol. So, with that in mind, I would suggest looking into Berberine or Inositol as a viable option instead of Metformin for PCOS.
I’m already taking Metformin. What should I do?

Make sure that you are also following a good PCOS diet and exercising to ensure that you are getting the maximum benefits.
You may want to consider some of the natural alternatives to Metformin and look at weaning off of it if you can.
What has your experience of Metformin been? I’d love to hear from you! Leave me a comment a let me know!
- sustainable pcos weight loss strategies
- Over 5500 women have done it and seen results
- [bonus] Done for you pcos meal plans
- [bonus] intermittent fasting for pcos course
- [BONUS] personalised nutrition plan
JOIN OVER 5,500 OTHERS
References
1Johnson, NP. Metformin use in women with polycystic ovary syndrome. ANNALS OF TRANSLATIONAL MEDICINE, 2014.
2Lashen, N. Role of metformin in the management of polycystic ovary syndrome. THERAPEUTIC ADVANCES IN ENDOCRINOLOGY AND METABOLISM, 2010.
3 Karimzedeh, MA; Javedani, M. An assessment of lifestyle modification versus medical treatment with clomiphene citrate, metformin, and clomiphene citrate–metformin in patients with polycystic ovary syndrome. FERTILITY AND STERILITY, 2010
4The Diabetes Prevention Program Research Group. Long-Term Safety, Tolerability, and Weight Loss Associated With Metformin in the Diabetes Prevention Program Outcomes Study. DIABETES CARE, 2012.
5Niemuth, NJ; Klaper, RD. Low-dose metformin exposure causes changes in expression of endocrine disruption-associated genes. AQUATIC TOXICOLOGY, 2018.
6MacLaren, RD; Wisniewski, K; MacLaren, C; et al. Environmental concentrations of metformin exposure affect aggressive behavior in the Siamese fighting fish, Betta splendens. PLOS ONE, 2018.
7Morley, LC; Tang, T; Yasmin, E; Norman, RJ; Balen, AH. Insulin-sensitising drugs (metformin, rosiglitazone, pioglitazone, D-chiro-inositol) for women with polycystic ovary syndrome, oligo amenorrhoea and subfertility. COCHRANE DATABASE OF SYSTEMATIC REVIEWS, 2017.
8Regidor, PA; Schindler, AE; Lesoine, B; Druckman, R. Management of women with PCOS using myo-inositol and folic acid. New clinical data and review of the literature. HORMONE MOLECULAR BIOLOGY AND CLINICAL INVESTIGATION, 2018.
9Facchinetti, F; Orrù, B; Grandi, G; Unfer V. Short-term effects of metformin and myo-inositol in women with polycystic ovarian syndrome (PCOS): a meta-analysis of randomized clinical trials. GYNECOLOGICAL ENDOCRINOLOGY, 2018.
10Wei, W; Zhao, H; Wang, A; et al. A clinical study on the short-term effect of berberine in comparison to metformin on the metabolic characteristics of women with polycystic ovary syndrome. THE EUROPEAN JOURNAL OF EDOCRINOLOGY, 2012.